What is The Best Method for Assessing a Casualty?

The best method for assessing a casualty in an emergency situation is to perform a quick primary survey followed by a more thorough secondary survey.
A primary survey is a quick assessment of a casualty to find and correct any life-threatening issues. It often follows a structure such as DR ABC (or DRSABC). This involves checking the following things:
- Danger – any hazards to yourself or bystanders?
- Response – is the casualty unconscious?
- Shout for help – if they are unconscious, shout for further help but do not leave their side
- Airway – open the airway by tilting the head back and lifting the chin
- Breathing – check for normal breathing for up to 10 seconds
- Circulation – perform CPR and use a defibrillator if the victim isn’t breathing
A primary survey should be carried out to assess all casualties.
Once a primary survey has been performed, you can move onto a more thorough secondary survey. It may not be possible to perform a secondary survey if there are problems with the primary survey. For example, performing CPR takes priority over performing a secondary survey.
The secondary survey involves:
- History – finding out the history of the incident / illness from the casualty or bystanders
- Examination – looking for visual clues
- Vital signs / observations – if trained, recording relevant observations
The primary and secondary survey provide a structure for you to assess each casualty in a logical way. You can learn how to perform primary and secondary surveys in more detail by signing up to a free online first aid class.
A Complete Head-to-Toe Examination
When conducting a secondary survey, you will perform a more thorough and vigorous examination of the patient. This is carried out in a structured head-to-toe sequence. We start at the head as injuries sustained here are most likely to be life-threatening, so identifying and treating them quickly is crucial.
A complete head-to-toe examination is an important part of a first aider’s role as it gives a clearer picture of a patient’s condition. By locating any injuries, assessing their vital signs, and detecting any concerns such as a concussion or shock, we can help medics prioritize treatment as quickly and effectively as possible once they arrive.
Always wear gloves during a head-to-toe assessment to lower the risk of cross-contamination and infection. If possible, make notes during your examination so that you can easily relay the information to the EMTs or ambulance personnel.
If the patient is conscious, you must ask permission before beginning a head-to-toe examination. If the patient is unconscious, permission is implied.
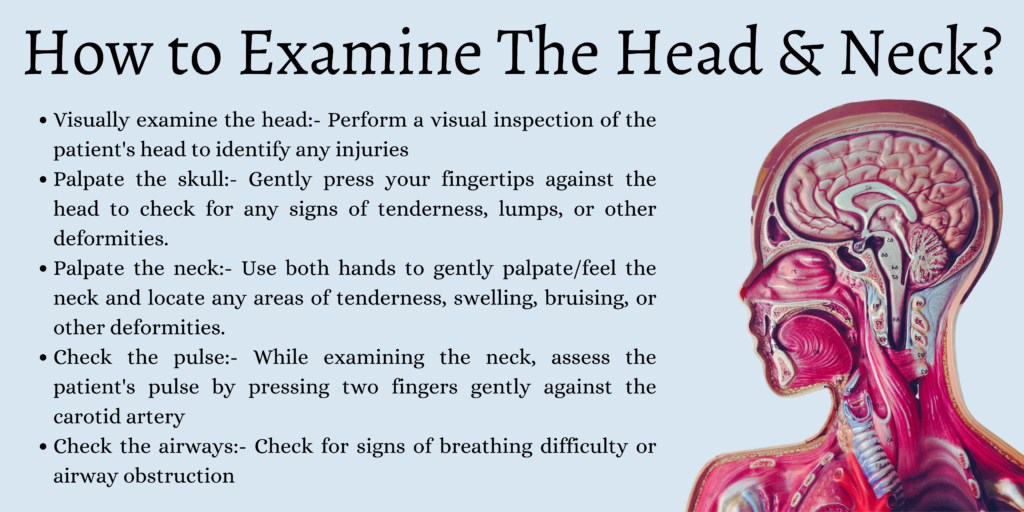
Examine The Head & Neck
Visually examine the head
Perform a visual inspection of the patient’s head to identify any injuries such as bruising, swelling, or lacerations. As you examine the head, check for any signs of active bleeding and, if found, work quickly to apply pressure to the wound to stop the blood flow.
Check for fluid from the ears and nose. Observe the nose for signs of breakage, and look inside the mouth for broken teeth, blood flow, and cuts.
During your examination of the patient’s head, you should also take note of the patient’s mental state and level of consciousness.
Palpate the skull
Gently press your fingertips against the head to check for any signs of tenderness, lumps, or other deformities. Pay close attention to the shape of the skull. Abnormal lumps, bumps, depressions, or other signs of asymmetry could indicate a serious injury, such as a fractured skull or swelling of the brain.
For more detailed information, read our guide to identifying the signs of a serious head injury.
Once you have conducted a thorough examination of the head, move on to the neck.
Palpate the neck
While supporting the head, use both hands to gently palpate/feel the neck and locate any areas of tenderness, swelling, bruising, or other deformities. Don’t forget to include the collarbone in your examination, paying particular attention to any areas of asymmetry.
Check the pulse
While examining the neck, assess the patient’s pulse by pressing two fingers gently against the carotid artery. If you’re unsure of how to do this, you can refresh your memory with our informative step-by-step guide here.
Check the airways
Check for signs of breathing difficulty or airway obstruction. If the patient is conscious, ask them to try swallowing and taking a deep breath, reporting any signs of difficulty or discomfort.
Important reminder: If you uncover an injury during a head and neck examination, you must seek emergency medical help immediately.
Examine The Chest
Visually examine the chest
Pay attention to any signs of injury or trauma, such as cuts and bruises. As the patient breathes in and out, observe how the chest rises and falls, paying attention to any areas that seem out of line or asymmetrical.
If the patient is conscious, ask them to take a couple of deeper breaths and to report any pain or discomfort.
Audibly examine the chest
If you have access to a stethoscope, use this to listen to the patient’s breath, noting any unusual sounds, such as wheezing and crackling, which can indicate damage to the lungs.
Next, use the stethoscope to listen to the patient’s heart rate and rhythm. Note down the beats per minute and pay attention to any irregularities, such as arrhythmias.
If you don’t have access to a stethoscope, you can still audibly examine the patient by pressing your ear to the person’s chest and listening to their breath unaided.
Palpate the chest
After visually and audibly examining the chest, use your hands to gently apply pressure to the rib cage area and check for signs of tenderness, injury, or deformity.
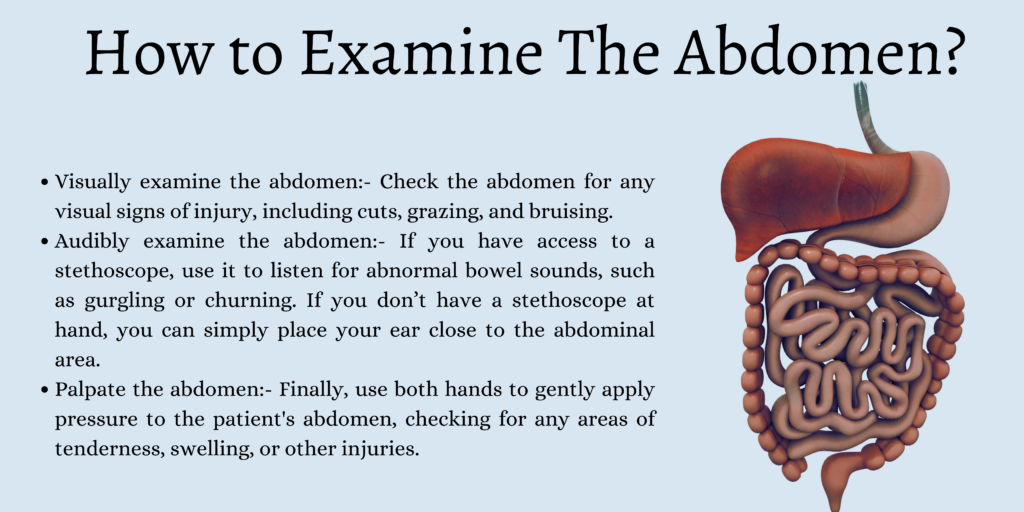
Examine The Abdomen
Visually examine the abdomen
Check the abdomen for any visual signs of injury, including cuts, grazing, and bruising. Check to see if the skin is a uniform color, and visually inspect the abdomen for signs of unusual swelling or distension, which could indicate a medical emergency.
Audibly examine the abdomen
If you have access to a stethoscope, use it to listen for abnormal bowel sounds, such as gurgling or churning. If you don’t have a stethoscope at hand, you can simply place your ear close to the abdominal area.
Palpate the abdomen
Finally, use both hands to gently apply pressure to the patient’s abdomen, checking for any areas of tenderness, swelling, or other injuries.
Locate the liver and spleen, which can be found under the patient’s right and left ribs. Feel for any swelling or enlargement, and pay particular attention to any spots of unusual hardness, which can be a sign of a medical emergency.
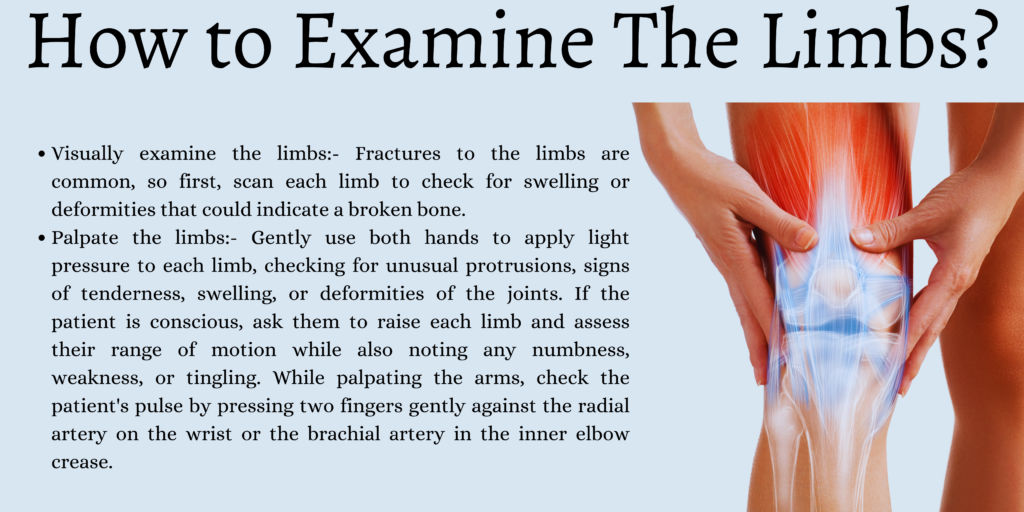
Examine The Limbs
Visually examine the limbs
Fractures to the limbs are common, so first, scan each limb to check for swelling or deformities that could indicate a broken bone. Also, scan each joint for possible signs of dislocation.
If the patient has active bleeding, quickly apply pressure to stop the blood flow and, using gloves, clean any open wounds to lessen the chance of infection.
Palpate the limbs
Gently use both hands to apply light pressure to each limb, checking for unusual protrusions, signs of tenderness, swelling, or deformities of the joints.
If the patient is conscious, ask them to raise each limb and assess their range of motion while also noting any numbness, weakness, or tingling.
While palpating the arms, check the patient’s pulse by pressing two fingers gently against the radial artery on the wrist or the brachial artery in the inner elbow crease.
Never apply pressure to an area where there is an obvious fracture, as this can make the injury worse. If you suspect a fracture is present, immobilize and support the limb by using a sling or a splint and seek immediate medical assistance.
Examine The Spine
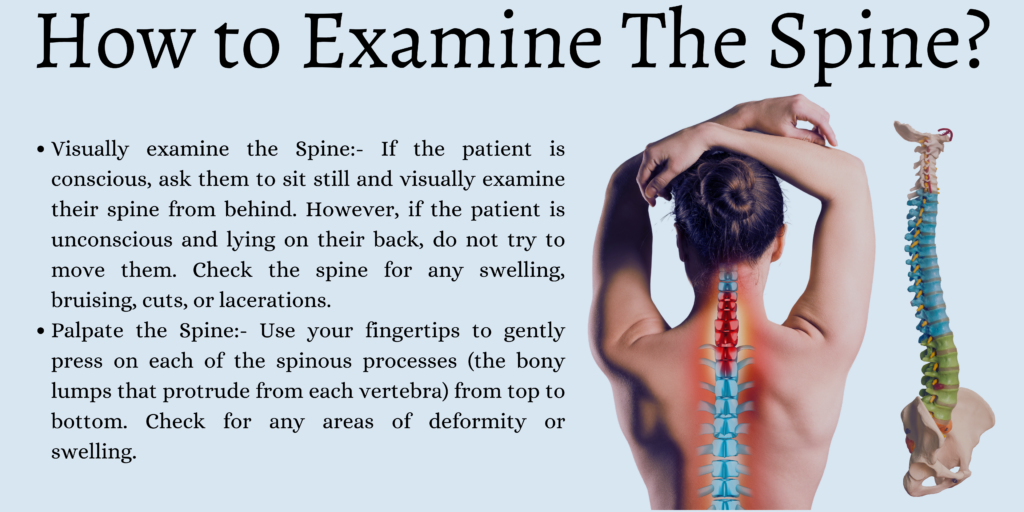
Visually examine the spine
If the patient is conscious, ask them to sit still and visually examine their spine from behind. However, if the patient is unconscious and lying on their back, do not try to move them.
Check the spine for any swelling, bruising, cuts, or lacerations. Also, pay attention to the curve of the spine and note any areas of asymmetry. If the patient is conscious, ask them to slowly move their head up and down and side to side while observing their range of motion and asking them to report any pain or discomfort.
Palpate the spine
Use your fingertips to gently press on each of the spinous processes (the bony lumps that protrude from each vertebra) from top to bottom. Check for any areas of deformity or swelling. If you suspect that the patient has a spinal injury, it’s essential to stabilize their head and neck and seek emergency medical assistance immediately. Do not try to move the patient, as this could lead to further irreparable damage.