What is the Difference Between Hypoglycemia and Hyperglycemia?
Hypoglycemia (low blood sugar) and hyperglycemia (high blood sugar) can both occur in patients who have diabetes. Diabetes occurs when the body does not produce enough insulin (known as ‘Type 1 Diabetes’) or the cells in the body stop responding to insulin (known as ‘Type 2 Diabetes’).
So what’s the difference between hypoglycemia and hyperglycemia? And how can a first aider spot the difference? Read on to find out how!
Hypoglycemia
Hypoglycemia occurs when insulin is in excess of that needed to balance the patient’s food intake and energy expenditure.
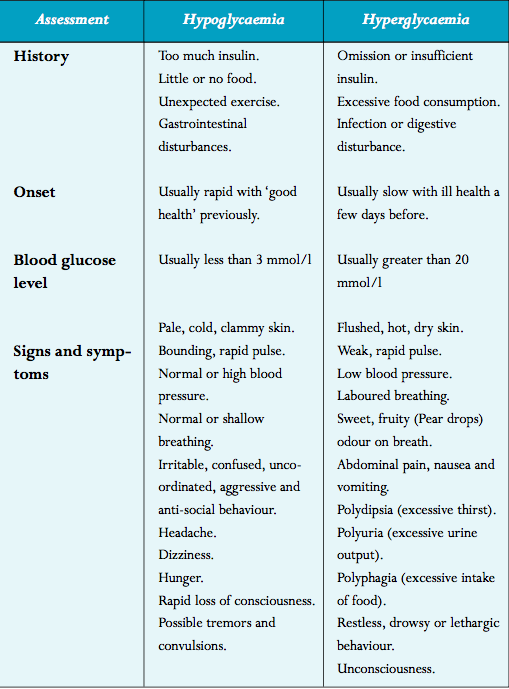
If untreated it will lead to unconsciousness and if prolonged, irreversible damage can occur. Signs and symptoms can be found for hypoglycemia and hyperglycemia in the table below.
Hypoglycemic patients may appear drunk although alcohol may also induce hypoglycemia. You should never discount the possibility that a patient who appears to be drunk may in fact be hypoglycemic. Most patients under the influence of alcohol will have their blood glucose levels recorded at hospital to ensure that they are not hypoglycemic.
Hyperglycemia
Hyperglycemia is often the presenting feature of diabetes. Patients who have not been diagnosed as diabetics will often go to their doctor complaining of excessive hunger, thirst and urination.
On testing their blood glucose levels they are often found to be greater than 20 mmol/l (normal non-diabetics range is 3.0-5.6 mmol/l).
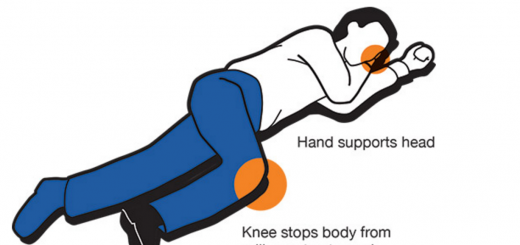
Diabetic patients who are hyperglycemic have often been ill for some hours or days and have since deteriorated − most calls for assistance are made when the patient falls unconscious
Want to learn more? Our advanced online first aid course contains information on diabetes and a range of other medical conditions.