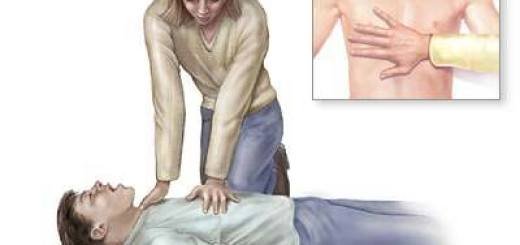
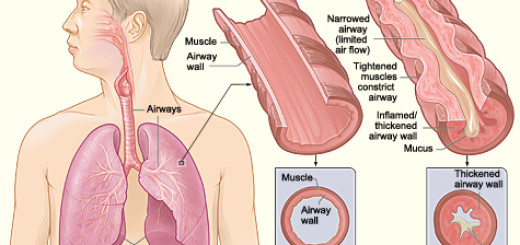
How to Measure and Record Vital Signs
Professionals in the medical field make use of vital signs in several ways. Whenever an individual’s vital signs vary from the normal results, it helps in assessing their overall health, thereby detecting the presence of any diseases.
Studying the vital signs also aids in monitoring if the treatment someone is going through is proving to be effective or not. When compared to many other medical tests, measuring a person’s vital signs is quite simple and requires medical equipment that’s not very high-tech.
Although the process of recording vital signs is straightforward, the data derived from it can help in saving someone’s life and treating them effectively.
What are Vital Signs?

Vital signs are measurements that help in checking a human body’s basic functions. They usually serve as the first step of every medical evaluation or examination. They help medical professionals detect the presence of any underlying conditions that could be affecting a patient’s health.
There are five main vital signs, and they are as follows:
- Body temperature
- Pulse/heart rate
- Blood pressure
- Vital Sign #3 Oxygen Saturation (SpO2)
- Respiratory/breathing rate
Vital Sign 1: Temperature
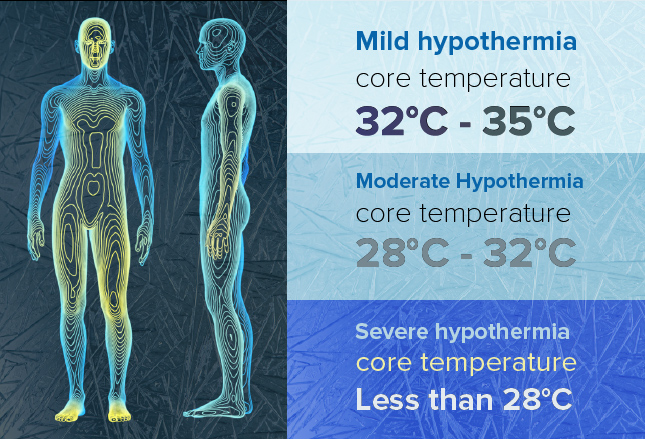
The body temperature of a person varies depending on factors such as:
- Gender
- Time of day
- Consumption of food and fluids
- Recent activities
Among women, it also depends on which stage of the menstrual cycle they’re at. A human being’s normal body temperature usually remains between 97.8° F (36.5°C) to 99°F (37.2°C).
Body temperature can be measured in the following ways:
- Orally
When you take someone’s temperature orally, you can either use a digital thermometer or a traditional glass thermometer.
- Rectally
When body temperature is measured rectally, it is normally about 0.5° F to 0.7° F higher than when it’s measured orally.
- Axillary
This is when a thermometer is placed under the arm, and these are often 0.3° F to 0.4° F lower than when it’s measured through the mouth.
- By skin
A special thermometer is often used to measure the temperature of a person’s skin on their forehead. There also exist certain thermometers that don’t require skin contact to measure body temperature.
- By ear
When one’s temperature is measured through the eardrum, it helps in determining their core body temperature.
Vital sign 2: Pulse rate
Taking a patient’s pulse is an important part of your physical assessment and secondary survey.
Whist you can obtain this information electronically, you should always start by feeling the pulse yourself as this will give you more information.
What are you looking for when taking the pulse?
The obvious answer to this question is the number of beats per minute or pulse rate but in addition you should be feeling the pulse to see if it is regular or irregular. An irregular pulse can be an indication of Atrial Fibrillation (A-Fib).
If you discover an irregular pulse, this should prompt you to ask your patient if they have any heart conditions, or if they have ever been told they have Atrial Fibrillation or A-Fib. A-Fib may cause no symptoms at all but does significantly increase the risk of a stroke.
Another important piece of information to note when taking a patients pulse is the quality or strength of the pulse. You should note if the patients pulse is any of the following:
Bounding
If the heart is pumping a large amount of blood with each heartbeat, the pulse will feel very strong. This strong pulse is called a “bounding” pulse
Weak or ‘thready‘
If the heart is pumping only a small amount of blood with each heartbeat, the pulse will be harder to detect. This type of pulse is called weak or thready. If the pulse is weak, you may have trouble feeling (palpating) the pulse at first.
What is the normal pulse rate?
A normal pulse in an adult is around 60 – 100 beats per minute (bpm).
Vital Sign 3: Blood Pressure (BP)
Every blood pressure reading consists of two numbers or levels. They are shown as one number on top of the other, for example 165/60. The first (or top) number is the systolic blood pressure. It is the highest level your blood pressure reaches when your heart contract.
The second (or bottom) number is the diastolic blood pressure. It is the lowest level your blood pressure reaches as your heart relaxes between beats.
How to record a manual blood pressure (BP)
To begin a manual blood pressure measurement, use a properly sized blood pressure cuff. Lightly press the stethoscope’s bell over the brachial artery just below the cuff’s edge.
Check for the patients pulse and inflate the cuff until the pulse stops. Add another 10-15 units on the pressure gauge. Checking the pulse during inflation prevents unnecessary discomfort caused by over-inflation of the cuff.
Listen with the stethoscope, slowly release the valve to maintain a slow deflation of the cuff and simultaneously observe the guage. When the pulse is heard in the stethoscope you have identified the patients systolic pressure.
Continue to deflate the cuff – when the pulse sound disappears you have identified the diastolic pressure.
Vital Sign 4: Oxygen Saturation (SpO2)
A pulse oximeter is a device intended for the non-invasive measurement of blood oxygen saturation (SpO2) and pulse rate.
Typically a pulse oximeter uses two LEDs (light-emitting diodes) generating red and infrared lights through a translucent part of the body. Bone, tissue, pigmentation, and venous vessels normally absorb a constant amount of light over time. Oxyhemoglobin and its deoxygenated form have significantly different absorption pattern.
The arteriolar bed normally pulsates and absorbs variable amounts of light during systole and diastole, as blood volume increases and decreases. The ratio of light absorbed at systole and diastole is translated into an oxygen saturation measurement.
The pulse oximeter should be placed on the patients finger. You should give the readings time to settle before taking note of the figures you are given. This can take anything from a few seconds to a minute or two depending upon a number of factors.
Normal oxygen saturation levels should be considered to be above 94% or 88% – 92% for a patient who has chronic lung disease.
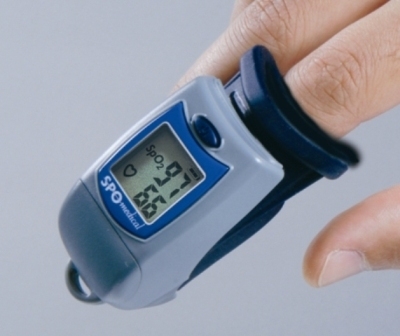
Vital sign 5: Respiratory rate
Normal respiration is an automated process and does not require conscious effort. However, in the case of illness or trauma, a patient’s respiratory rate may become unusually fast or slow indicating the need for immediate medical attention.
The respiratory rate is simply the number of breaths an individual takes per minute.
Observe and count the rise and fall of the patients chest over a period of time. Count the number of breaths in 15 seconds and multiply by 4, 20 seconds and multiply by 3, 30 seconds and multiply by 2 or observe for a full minute.
Try to count the respiratory rate discreetly to gain a more accurate reading. Also be aware of patient dignity when counting the respiratory rate of a female patient. An ideal way to obtain the respiratory rate of a female is to do so whilst taking the patients pulse as this will prevent any awkwardness.
What are Normal Respiratory Rates?
Respiratory rates, like pulse rates, will vary with the patient’s age.
Adult: 12 – 20 breaths per minute
Child: 15 – 30 breaths per minute
Infant: 25 – 50 breaths per minute
What to Do Before Measuring Your Blood Pressure?
Keep the following points in mind while measuring your blood pressure at home:
- Go to the bathroom before you sit down to record the reading.
- Don’t consume caffeine or smoke for about 30 minutes before measuring your blood pressure.
- Make sure you’re relaxed at least five minutes prior to taking your blood pressure.
- Jot down the time and date of each blood pressure reading.
- Measure your blood pressure at the same time every day or as per doctor’s instructions.
- Take more than one reading. Keep them a minute apart and record them all.
- Be sure to take your blood pressure records the next time you visit your doctor.
- While measuring your blood pressure, ensure that your back is supported, place your feet uncrossed on the floor, and keep your arm on a flat surface, such as a table. The upper part of your arm should be kept at the same level as your heart.
If you notice multiple high blood pressure readings, contact your healthcare provider. In case you have a diastolic or systolic reading that is higher than usual, contact the emergency medical services.
Why Should I Monitor My Blood Pressure at Home?
When someone suffers from high blood pressure or hypertension, monitoring their blood pressure at home enables your doctor to keep track of how much your blood pressure changes from one day to the next and even throughout the day.
It also helps them understand if the medication they take for their blood pressure is working effectively or not.
Equipment Needed to Measure Blood Pressure
The following can be used to measure one’s blood pressure at home:
- Aneroid blood pressure monitor
Comes with a dial gauge, and one can look at the pointer to determine the readings.
Equipped with a small screen that displays the blood pressure reading.
Regardless of the device you go for, ensure that the cuff properly fits your arm because if it’s too small or too big, it can display inaccurate numbers. Remember not to measure someone’s blood pressure on a leg or an arm that has suffered injuries to the tissue or is currently severely injured.
Health Implications of Abnormal Vital Signs
Let’s take a look at the various health implications of abnormal vital signs.
Health Implications of Abnormal Body Temperature
The following could be the reasons behind abnormal body temperature:
- Fever
- Illness caused due to heat
- Cancer
- Autoimmune disease
Health Implications of Abnormal Respiratory Rate
The health implications associated with abnormal respiratory rate:
- Use of narcotics or alcohol
- Dehydration
- Infection or fever
- Sleep apnea
- Drug overdose
- Lung disease
- Metabolic issues
- Head injury or stroke
- Anger, panic, or stress
Health Implications of Abnormal Pulse
If you have a slow pulse, it could mean:
- Sinus node dysfunction
- Heart block
A rapid pulse could indicate:
- Situations that cause one’s heart to beat faster, such as stress or exercise
- Heart arrhythmia
Health Implications of Abnormal Blood Pressure
Abnormal blood pressure might indicate:
- Infections
- Heart problem
- Anemia
- Dehydration
- Certain medicines
FAQs
1. What are the different vital signs?
There are four vital signs, and they are body temperature, pulse, blood pressure, and respiratory rate.
2. What is considered as normal body temperature?
Normal body temperature usually ranges between 97.8 F to 99 F.
3. What should be the blood pressure reading of a healthy person?
The blood pressure reading of a healthy person is 120/80 mm Hg.
4. Can blood pressure be measured at home?
Yes, blood pressure can be measured at home.
Conclusion
The vital signs of a person can vary on the basis of factors such as:
- Gender
- Age
- Weight
- Activity levels
A doctor can determine what the respective vital signs indicate depending on these factors. However, people in the medical community keep a certain standard of what is normal regarding vital signs readings.
Suppose they notice a significant difference between the reading of a patient’s vital signs from what is normal in terms of a healthy individual. In that case, that’s when they know that medicines or treatments need to be administered.