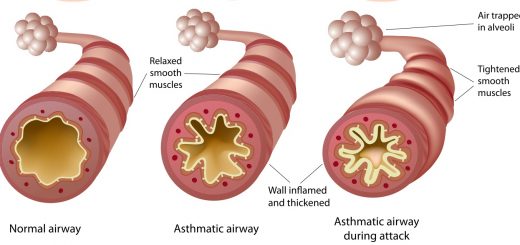
How Does The Heart Beat By Itself?
The heart requires a rhythm in which to pump the blood, this rhythm allows time for blood to fill the ventricles and for the ventricles to empty completely before filling again. In patients with an abnormal rhythm, incorrect filling and emptying occurs which can cause chest pain and shortness of breath as less oxygenated blood is delivered to tissues.
The heart has its own electrical pacing system to regulate the heartbeat. The areas of the heart responsible for co-ordinating the electrical activity of the heart are:
- The sinoatrial node
- The atrioventricular node
- The Purkinje fibres
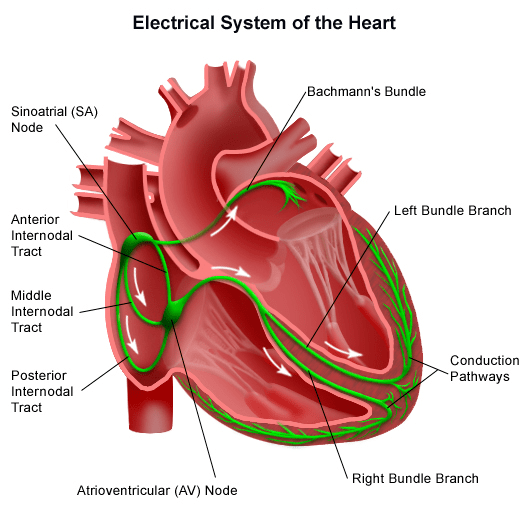
The electrical flow starts in the sinoatrial node (which acts as an ignition switch) spreading across both atria to the atrioventricular node. This means that the atria contract before the ventricle squeezing blood into the ventricles.
The electrical flow then spreads down an isolated path between the two ventricles called the Purkinje fibres to the bottom of the ventricles to ensure the bottom segment of the ventricles contracts before the top, this is critical to ensure the whole ventricle is emptied.
Problems occur when there is disruption to the electrical pathway, creating an abnormal rhythm which is often referred to as an arrhythmia.
A common arrhythmia is atrial fibrillation (AF / A-Fib). Atrial fibrillation is a condition where there is disorganised electrical activity in the atria. This then leads to disorganised flow through the sinoatrial node which fires irregularly.
Patients with atrial fibrillation often have medication to control the rate of the heart beat (which is often faster) and rhythm control (medication that can partially block the electrical flow).
Due to the disorganised electrical activity in the atria, the blood flow is also disorganised in the atria. This can cause an increased risk of clot formation. Patients with atrial fibrillation are often on blood thinning tablets to decrease the risk of a stroke or thrombosis from a blot clot arising from the atria.