What is hypovolemic shock?
Hypovolaemic circulatory shock is a clinical state in which blood supply to the body’s tissues is rendered inadequate by loss of blood, fluid or the loss of plasma in burns.
It may be caused by:
- Blood loss from the body (external or internal bleeping).
- Fluid loss from the body, as in burns, or severe vomiting and diarrhoea.
- Failure of the heart pump.
- Sudden dilatation of blood vessels as in anaphylaxis.
A reduction of the blood volume leads to a fall in pressure in the arteries and arterioles. This triggers response from the sympathetic nervous system, which releases epinephrine/adrenaline-like substances. The effect is to cause the pulse to rise and the arterioles to constrict, resulting in skin pallor and a fast, weak pulse. Pain and anxiety can exaggerate this response.
The raised pulse rate leads to a need for the heart to work harder and thus an increased demand for oxygen by the heart muscle. This will now be possible if the shock is not controlled.
Blood flow to the skin and periphery is reduced in an effort to preserve blood supply to vital organs such as the brain, heart, liver and kidneys.
In healthy young adults, the pressure in the arteries is usually maintained despite considerable blood loss as a result of the epinephrine/adrenaline release but in casualties with heart disease, there is a much earlier fall in pressure as the heart muscle fails earlier.
Recognition of hypovolemic shock
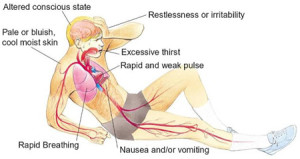
Signs and symptoms of hypovolemic shock are:
- Skin pallor with cold clamminess – due to constriction of the peripheral blood vessels as a result of epinephrine/adrenaline release.
- Raised pulse rate – due directly to adrenaline release.
- At a later stage, reduced pressure in the arteries – due to loss of circulating fluid.
- Confusion, aggression and drowsiness – due to cerebral hypoxia.
- Raised respiratory rate – due to hypoxia.
- General weakness – due to hypoxia.
- Thirst – due to loss of circulating fluid volume.






thanks for the facts.