First Aid for Emergency Childbirth
Medical emergencies can happen at any given time, and an emergency childbirth falls under the same category. One could find themselves in a situation where it’s required for them to help a woman who is about to give birth.
Since childbirth is a natural process, the body knows exactly what to do, and the responsibility of a bystander in this situation is to provide reassurance and comfort to the pregnant woman. It’s also vital to provide them with all the things they need at that moment, such as cushions, blankets, water, and so on.
Unexpected events that lead to emergency childbirth could include natural disasters, traffic, malfunctioning elevators, and even women going into labor while on a flight.
In normal circumstances, childbirth happens in an ambiance that has been selected by the mother beforehand, around a team of medical professionals. This could be at a hospital, at home, or at a birthing center.
However, when emergencies present themselves, childbirth happens in an unplanned manner till the medical services arrive to handle the situation. In this article, we will be discussing how to prepare for an emergency childbirth, what are the different stages of labor, and so on.
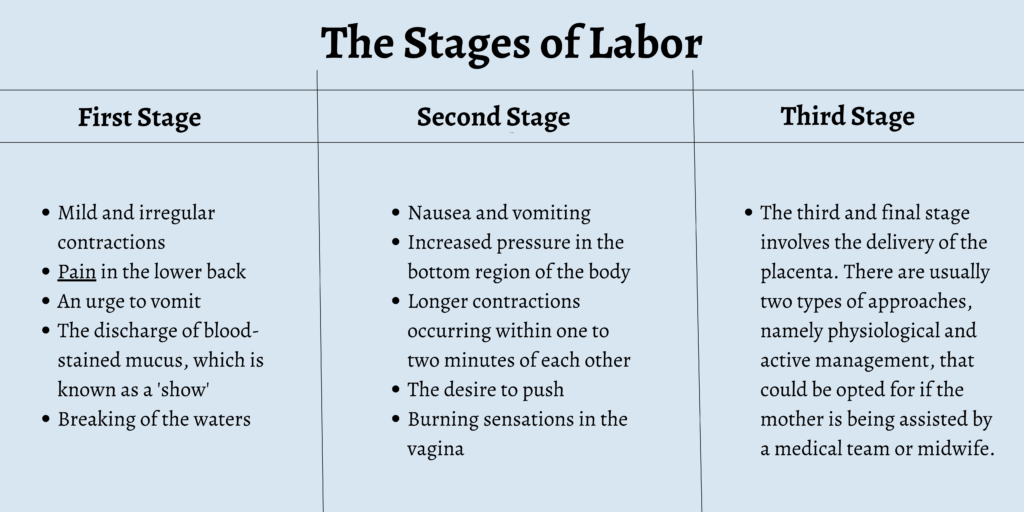
The Stages of Labor
Labor is divided into three stages. They are as follows:
First Stage
The first stage of the labor is when the mother’s cervix begins to soften and open up. This stage can further be divided into an early stage and an active stage. During the early stage, the woman’s cervix dilates, and they can experience:
- Mild and irregular contractions
- Pain in the lower back
- An urge to vomit
- The discharge of blood-stained mucus, which is known as a ‘show’
- Breaking of the waters
As a woman’s body prepares to give birth, they can do the following things to experience some form of comfort during early labor:
- Go for a walk
- Switch positions
- Play some relaxing music
- Try out the breathing exercises they learned during childbirth classes
- Take a shower
- Have snacks so that their body has enough energy
The active stage entails the cervix dilating further and reaching up to 10 cm. The mother could experience stronger and more painful contractions, and this is when their water will break if it hasn’t already.
Experiencing leg cramps and pressure in one’s back is common, too, during this stage. Active labor can last up to eight hours or longer.
Second Stage
The second stage is when the actual delivery takes place. The signs that accompany this stage include:
- Nausea and vomiting
- Increased pressure in the bottom region of the body
- Longer contractions occurring within one to two minutes of each other
- The desire to push
- Burning sensations in the vagina
When it’s time for the mother to push the baby out, they can try out different positions till they find one that’s the most comfortable. Assisted delivery might be required if the mother can’t push effectively due to exhaustion. Once the baby comes out, the airway needs to be cleared immediately.
Third Stage
The third and final stage involves the delivery of the placenta. There are usually two types of approaches, namely physiological and active management, that could be opted for if the mother is being assisted by a medical team or midwife.
When an emergency childbirth is involved, the third stage entails waiting for the placenta to be expelled, which is often accompanied by further contractions. After the placenta is delivered, the mother’s uterus should be cleaned to remove any remaining fragments, as it aids in keeping infections and bleeding at bay.
Importance of Knowing First Aid for Emergency Childbirth
Being aware of the first aid involved in emergency childbirth allows one to take care of the pregnant woman, making sure that the surroundings are safe and hygienic. The ones who know about emergency childbirth will be aware of the following pointers:
- Protecting the mother is just as crucial as providing her with emotional support.
- Even if a woman’s water has broken, she should have enough support to shift into the positions that make her comfortable.
- Before helping the woman, make sure to get her consent. This includes initiating any kind of physical contact.
- If there are any bystanders who aren’t helping the process, ask them to clear the area.
- Put on gloves and place clean towels and blankets under the woman. Since many women could feel embarrassed or shy in such circumstances, use a clean towel or sheet to cover their abdomen.
Knowing When to Seek Help
Knowing when to seek help by contacting a midwife or hospital is extremely vital. Call for help in case:
- The woman’s contractions are regular, and there are about three of them every 10 minutes
- The mother’s water breaks
- The contractions are too strong, and the woman needs pain relief
- While helping a woman with emergency childbirth, it’s important to remember the following:
- Make sure the pregnant woman does not leave to use the bathroom, as she could end up delivering the baby on the toilet.
- No one should attempt to physically delay the delivery in any manner, as it could harm both the child and the mother.
- Do not touch the woman anywhere without her consent, including her vagina, legs, and arms.
- Ensure you do not grab the baby too hard.
Preparing for Emergency Childbirth
Expecting mothers should be prepared for any possible situation when it comes to giving birth because them staying prepared is more crucial than the ones around them being ready for childbirth emergencies.
As you inch closer to your due date, keep a list with you at all times that includes the numbers of those who can help. Make sure the family car is filled with fuel, and if you go into labor sooner than predicted, your doctor or midwife should be contacted immediately.
Call 911 if you cannot reach your healthcare provider. In order to prepare the room for childbirth, one should use a shower curtain to cover the bed and place a clean sheet over it. Keep your emergency kit near your bed for such extreme situations.
The supplies required for emergency childbirth depend on the stage in question. The things needed during labor and to prepare the bed include:
- Large underpads
- Bath towels
- Hand sanitizer
- Disposable gloves
- Large sanitary napkins
- Flashlight
The items required while the woman is giving birth are:
- White shoelaces to help in cutting the umbilical cord
- Scissors
- Large garbage bags
- Two plastic bags
- A big bowl
The person helping with the birth or staying with the mother before and during birth should remember a couple of things:
- Keep some towels under the pregnant woman that will help in catching the fluid after her water breaks. This is also necessary for any vaginal bleeding that could happen during labor.
- The stage where the mother is pushing the baby out could last for an hour or two if it’s the woman’s first child.
- Once the baby’s head comes out, feel the area around it in case the umbilical cord is around the child’s neck. The cord is slippery and has a jelly-like texture.
- After the baby’s shoulders come out, the rest of their body will come out soon as well.
- In case the child’s shoulders do not come out, ask the mother to lie on her back. By pulling her knees up towards her chest, she should then be asked to push.
What to Do After the Baby is Born
- After the baby is born, hold the head in a manner such that the fluid gets drained from the throat and nose.
- By placing the baby on the bare chest of their mother, cover both the baby and the mother with dry blankets. Put a hat on the child.
- Don’t hold the newborn upside down or spank them. Instead, rub their back if they aren’t breathing properly or crying.
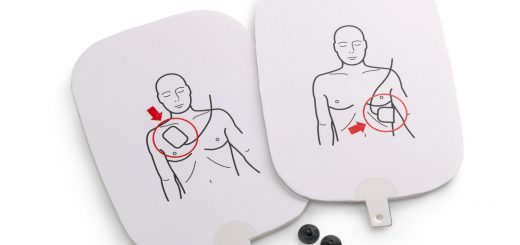
- If the baby still doesn’t breathe, start infant CPR.
A baby’s color is usually blue after they are born, and once they start crying, their color will eventually look normal. It is essential to keep the baby warm during this time, which is why covering them with a warm blanket is imperative.
Even if the mother does not plan to breastfeed, put the baby on the mother’s chest. This is done to prevent the mother from bleeding too much and also to provide the child with the food it requires right away.
The Umbilical Cord
The umbilical cord will pulsate even after the baby is born. Make sure not to pull the cord tight or cut it till it stops pulsating. Since the cord doesn’t possess any nerve endings, neither the mother nor the newborn will be hurt when it’s cut.
Here’s how you should cut the umbilical cord:
- Wash your hands thoroughly, put the gloves on, and keep the scissors and white shoelaces next to you.
- Tie one of the shoelaces around the umbilical cord almost three inches from the tummy of the child using a double knot.
- Use the other shoelace to tie it around the cord, making sure it’s about two inches away from the first one.
- Pick the scissors using the handle and cut between the tied knots.
- The end of the cord attached to the placenta of the mother should be placed into the bowl. Proceed to cover the baby and keep them warm.
The mother should breastfeed during the first hour after the child is born and every two hours until the milk comes in. This milk also helps in keeping the child away from any infections.
Even if the mother cannot access a medical facility or birthing center after an emergency childbirth, ensure that they go to the bathroom within an hour of their delivery.
Having vaginal discharge after giving birth is extremely natural. The discharge is known as lochia and can also contain blood for the first three days after your delivery. New mothers should remember to:
- Wash their hands before and after they breastfeed
- Keep their nipples and breasts dry and clean
- Wash their hands and sanitize after using the toilet and before and after changing pads
- Take a bath every day to keep the perineal region clean
- Change their pads at regular intervals throughout the day
Conclusion
The natural process of childbirth can last up to several hours, thereby allowing one enough time to contact a midwife or shift the pregnant woman to a birthing or medical facility. However, certain cases lead to the woman delivering in places that are nowhere close to what was originally planned.
In such circumstances, the responsibility of bystanders and first aiders is to provide help and support to the woman. Learning about the things to arrange for, how to comfort the mother, and how to handle the baby once it’s born enables you to create a soothing atmosphere for both the mother and the child.
FAQs
1. What are some of the items needed during emergency childbirth?
Some of the things needed during emergency childbirth include disposable gloves, scissors, hand sanitizers, bath towels, sanitary napkins, and underpads.
2. What to remember as a bystander during emergency childbirth?
Some of the things to remember as a bystander during emergency childbirth are to make the environment safe and hygienic for the mother, to not touch the woman anywhere without her consent, and to ask any other bystanders to clear the area.
3. How to look after a newborn following an emergency childbirth?
Make sure to wrap the baby in warm blankets and rub their back if they are not crying or have any trouble breathing. Bring them to their mother’s chest so they can be breastfed.
4. What are the two types of labor involved during the first stage of labor?
The two types of labor involved during the first stage of labor are early labor and active labor.
5. What are the two ways to manage the third stage of labor?
The two ways to manage the third stage of labor include active management and physiological management.





it is always a good idea to provide some sensible Aid to anyone who is in difficulty, thank you for your Training